FTC disclaimer: This post may contains affiliate links and we will be compensated if you click on a link and make a purchase.
Rheumatoid arthritis (RA) is a chronic autoimmune and inflammatory disease that predominantly attacks the joints, leading to pain, swelling, and potential loss of function.
In the UK, RA affects approximately 1% of the population, reflecting its significant impact on public health.
The aim of this article is to demystify RA by providing a comprehensive understanding of its symptoms, causes, and the effects it has on the body.
To ensure the accuracy and reliability of the information presented, we draw upon evidence-based data and reputable sources like the National Institute for Health and Care Excellence (NICE) and the Mayo Clinic.
Understanding RA is crucial for patients, healthcare providers, and the wider community to foster better management and support for those affected by this debilitating condition.
Symptoms and Impact on Daily Life
Rheumatoid arthritis (RA) is a chronic inflammatory disorder that primarily affects joints, but can also damage a range of body systems.
People with RA may experience tender, warm, swollen joints, often accompanied by stiffness that can be pronounced in the mornings or following periods of inactivity. Beyond the physical discomfort, RA often brings fatigue, which can profoundly impact daily life and well-being.
The burden of these symptoms can be substantial, encroaching upon every facet of life. Individuals living with RA report that their condition can make simple tasks like opening jars or tying shoelaces challenging.
Adaptations such as using assistive devices and engaging in energy conservation strategies become essential for maintaining independence and managing the disease’s impact on activities of daily living.
Personal accounts reflect the varied ways in which RA can affect one’s quality of life. Some individuals describe the need to “dose their activities” or adopt new strategies to cope with the limitations imposed by the condition, often grappling with feelings of helplessness and uncertainty that can lead to mood changes and social withdrawal.
Causes of Rheumatoid Arthritis
Rheumatoid arthritis (RA) is a complex disease influenced by a tapestry of genetic and environmental factors. At its core, RA is an autoimmune condition where the immune system mistakenly attacks the synovium—the lining of the joints—leading to inflammation and joint damage.
This battle within can spill over, affecting other body parts such as the heart and lungs. The exact trigger of this immune response remains a medical mystery, but what’s clear is the intertwining of genes and lifestyle.
Individuals with certain HLA class II genotypes may have a predisposition to RA, especially when environmental factors like smoking or obesity enter the fray, potentially igniting the disease or exacerbating its severity.
The genetic component doesn’t act alone; it’s more of a key that may unlock a reaction to environmental elements, such as infections that could set the immune system on an erroneous path.
The result is an unwarranted inflammatory onslaught on the joints, hallmarking RA as an affliction where the body’s defense mechanism paradoxically turns into its adversary.
Understanding this interplay between genetics and environment is pivotal for grasping the causes of rheumatoid arthritis and tailoring effective interventions.
Effects of Untreated Rheumatoid Arthritis
When Rheumatoid Arthritis (RA) sidesteps treatment, it embarks on a destructive path that can substantially alter one’s health landscape.
The joints, those intricate intersections of movement, become battlegrounds for inflammation, leading to long-term damage such as fibrous tissue formation and bone fusion.
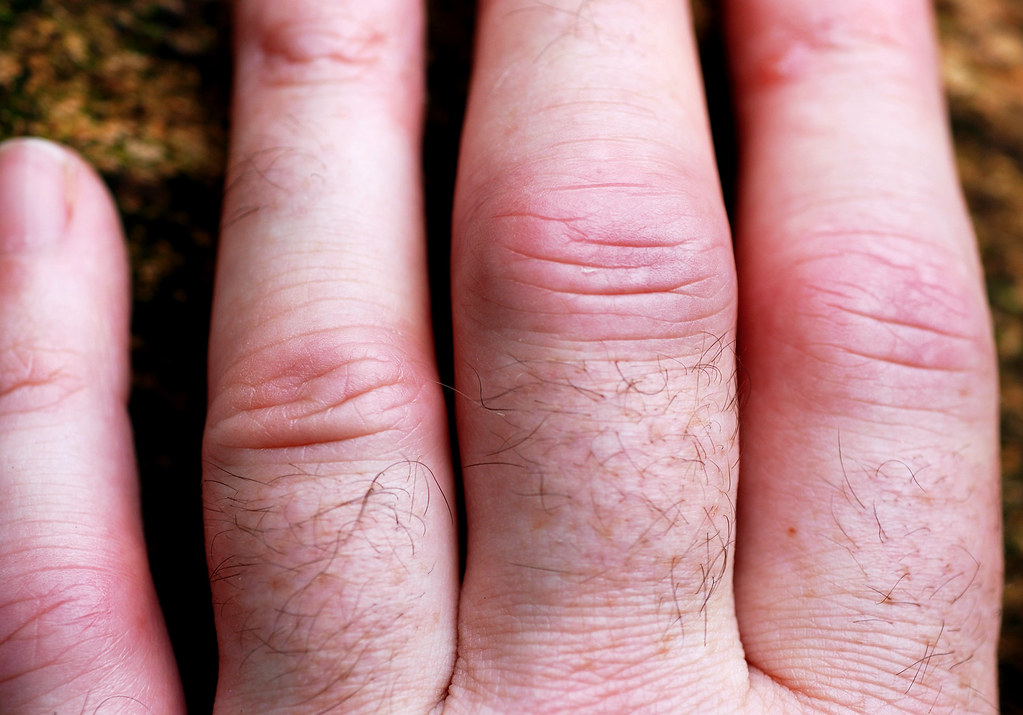
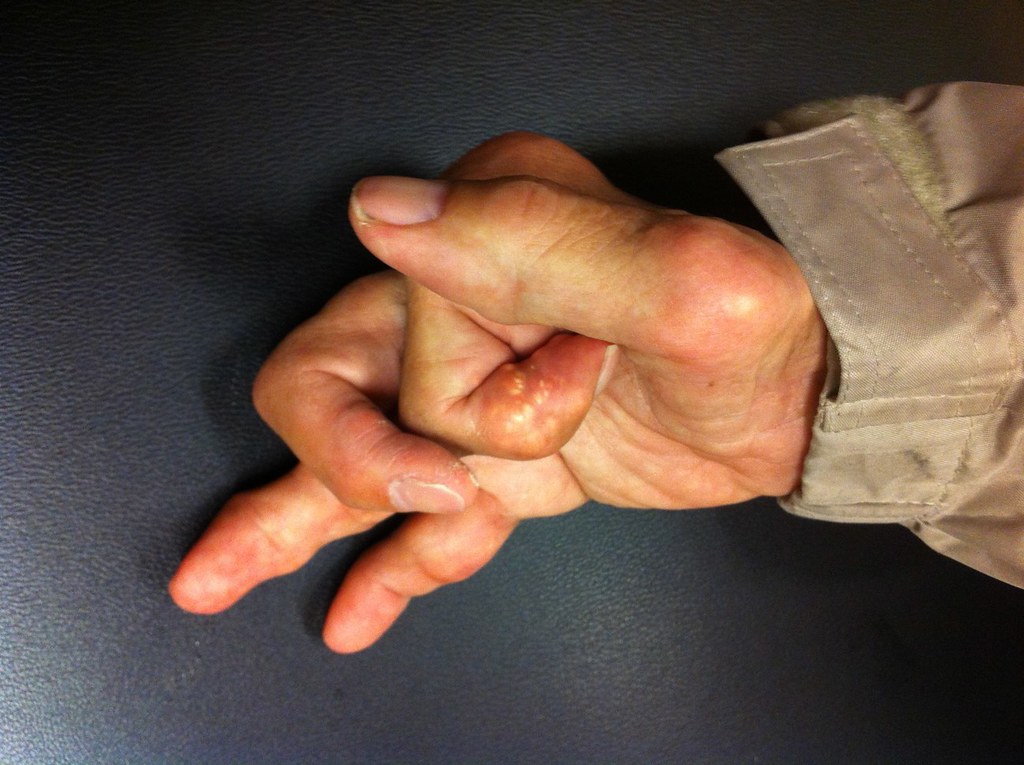
This relentless assault by one’s own immune system can manifest as deformity and reduced mobility, particularly in the hands, causing profound impacts on daily living.
Moreover, RA’s reach extends beyond the joints, increasing the risk of serious conditions like cardiovascular disease.
Inflammation can narrow blood vessels, setting the stage for blockages and heightening the chances of heart attacks or strokes. As such, early detection and management of RA are paramount.
Effective treatment not only curtails joint damage but also mitigates the elevated risks of associated health complications, safeguarding both quality and longevity of life.
Diagnosis and Treatment Options
Pinpointing rheumatoid arthritis (RA) involves a blend of blood tests and a physical examination.
Blood tests like the erythrocyte sedimentation rate (ESR) and C-reactive protein (CRP) assess inflammation, while a complete blood count (CBC) can reveal anemia common in RA. Imaging tests, such as MRI and ultrasound, may detect early joint damage.
Treatment options for RA are multifaceted, including medications like NSAIDs and disease-modifying antirheumatic drugs (DMARDs), physical therapy to maintain joint flexibility, and potentially surgery to correct joint damage.
A personalized treatment plan is crucial, tailored to individual symptoms and lifestyle. Regular consultations with healthcare providers ensure the most effective management of RA, minimizing its impact on daily life.
Lifestyle Changes and Complementary Treatments
Managing rheumatoid arthritis (RA) isn’t just about the medication and medical procedures; it’s also about tweaking your lifestyle to reduce symptoms and improve joint motion. To keep the gears of life well-oiled, here are some shifts that one can consider:
- Engage in regular physical activity – Exercise can strengthen the muscles around your joints, increase flexibility, and reduce fatigue. Think of it like oiling a squeaky hinge – a bit of movement can go a long way.
- Embrace weight loss – If you’re carrying extra pounds, shedding them can take some of the strain off your joints, like taking a load off a weary camel’s back.
- Optimize your diet with supplements – Ingredients like omega-3 fatty acids and Vitamin D might be helpful pals in this journey. However, always consult with healthcare providers for medical advice before starting any new supplement.
Additionally, there’s a world of complementary treatments to explore, from acupuncture to massage therapy.
They’re like the sidekicks to your superhero treatments, offering support where needed. Remember, while these lifestyle changes and therapies can be beneficial, they should complement, not replace, the treatment plan prescribed by your rheumatology team.
Before embarking on any lifestyle or treatment adventure, having a chat with your doctor is a must – think of it as getting the map before a treasure hunt. Together, you can determine the most suitable changes for you, ensuring that every step taken is a step toward better health.
Support for Those Living with Rheumatoid Arthritis
Living with rheumatoid arthritis can be a profound challenge, not only physically but emotionally as well.
Acknowledging the importance of emotional support, individuals grappling with this condition need not face it in solitude.
Moreover, an array of support groups and online communities present a valuable lifeline, offering shared experiences and coping strategies. These platforms, alongside professional emotional factors counseling, can significantly alleviate the feeling of isolation.
- Seek out patient-led support groups and online forums for shared experiences.
- Consider occupational therapy to assist in adapting to daily life with RA.
- Explore the potential for financial assistance through reputable sources.
It is essential for patients to remember: you are not facing this alone. Medical professionals, alongside a supportive community, are there to help navigate the complex journey of living with rheumatoid arthritis.
Conclusion
Rheumatoid arthritis (RA) is more than just a joint condition; it’s a systemic autoimmune disease that can significantly impact quality of life.
From morning stiffness and joint pain to potential effects on the skin, eyes, and internal organs, RA presents a complex challenge for patients and healthcare providers alike. Understanding the nuances of this disease, including its symptoms, causes, and progression, is vital for early detection and management.
While there is currently no cure, advancements in treatment have transformed many patients’ lives, providing relief and preserving function.
Prompt medical attention for symptoms and a proactive approach to care are crucial. If you suspect you may have RA or are managing the disease, seeking medical advice and support can pave the way to a more comfortable and active life.